Severe Abdominal Pain Could Be Sign of HAE, Case Study Reports
Written by |
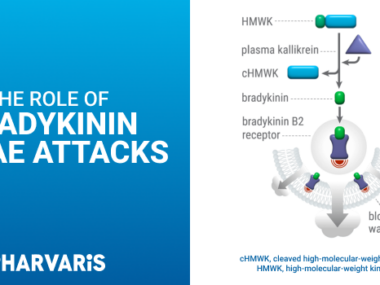
Hereditary angioedema (HAE) can present itself as a sudden and severe abdominal pain, even in the absence of other typical symptoms, such as swelling in the skin and mucosal linings, a case study from Japan has found.
According to the authors, physicians should not overlook these uncharacteristic symptoms and confirm HAE through a differential diagnosis (the process of the process of ruling out conditions that share similar symptoms).
The report, “Recurrent Acute Abdomen as the Main Manifestation of Hereditary Angioedema,” was published in Internal Medicine.
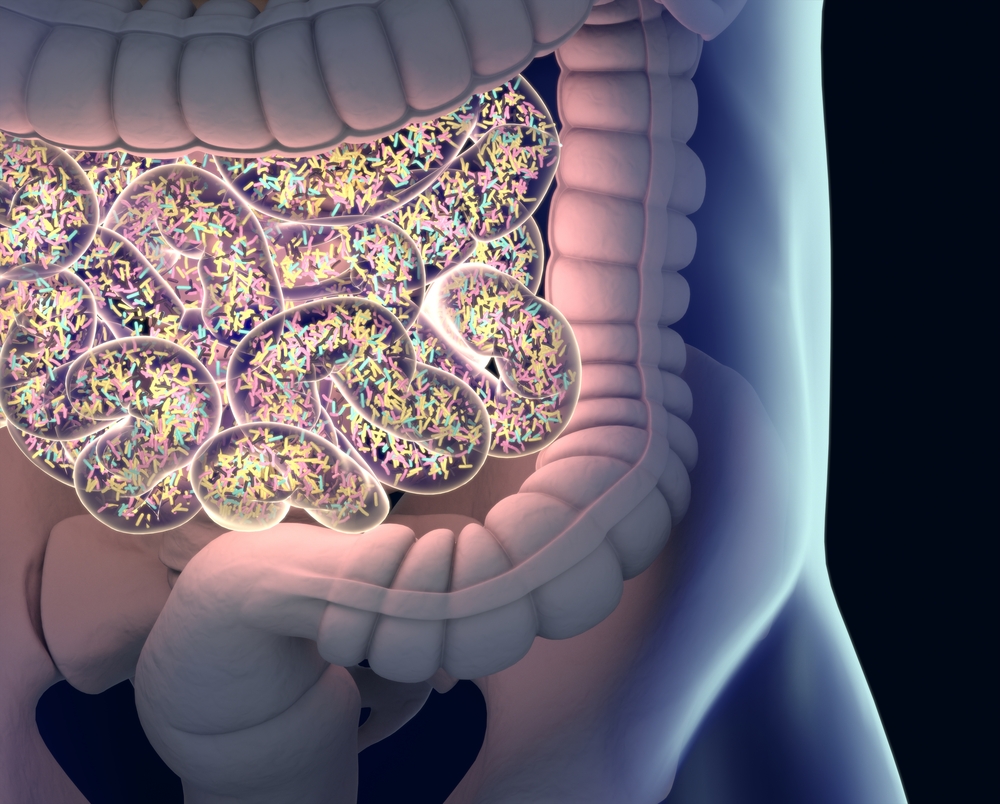
HAE is a rare genetic disorder characterized by sudden and recurrent episodes of swelling in the deeper layers of the skin, the upper airway, and the gastrointestinal (GI) tract. When angioedema flare-ups occur near the body surface, they are easily noticeable. But these signs can be overlooked when the main region affected is the GI tract.
In this case study, researchers described the case of a 45-year-old woman who had a recurrent 10-year medical history of severe abdominal pain accompanied by minor episodes of skin swelling in the hands and legs.
When she was 42, the patient underwent a panhysterectomy — surgery to remove the uterus and cervix — because physicians suspected endometriosis was to blame for the patient’s extreme abdominal pain.
However, after the procedure, the pain did not subside. In fact, it worsened to the point where the patient had to be brought to the hospital emergency department.
After a physical examination, physicians found no sign indicative of swelling (edema) under the skin, but the patient’s abdomen was slightly distended and tender to the touch. A computed tomography (CT) scan of the abdomen revealed a submucosal (a moist layer that lines many organs in the body and aids in the absorption and secretion of substances) edema of the ileum (the final section of the small intestine).
Concerned with the possibility of hereditary angioedema, physicians performed an additional blood test to measure the levels of C1-inhibitor — a protein encoded by the SERPING1 gene, whose mutations are a direct cause for types 1 and 2 HAE.
Test results revealed the patient suffered from C1-inhibitor deficiency directly associated with a genetic mutation in the SERPING1 gene, which accounts for 85% of all cases of type 1 HAE, and the patient was finally diagnosed with type 1 HAE.
She was prescribed with tranexamic acid (brand name (Cyklokapron) and on-demand therapy of plasma-derived C1-inhibitor concentrate to control her recurrent abdominal pain.
“The present case highlighted two critical clinical issues. [First], HAE can be overlooked if the main attacks involve only the gastrointestinal tract, and [second,] overlooking HAE can increase the risk of mortality in the patient as well as in any blood relatives,” researchers wrote.
“Our patient’s mother died from asphyxiation from the larynx following upper endoscopy before our patient was diagnosed with HAE,” they added. “Recently, one of her sons reported having occasional abdominal pain. The prophylactic [preventative] administration of [C1-inhibitor] concentrate before dental procedures, endoscopy, and endotracheal intubation is advised if C1-INH deficiency is diagnosed,” they added.