Angioedema diagnosis
Angioedema is characterized by swelling, or edema, in the tissues underneath the skin that can usually be diagnosed by a doctor after examining the affected area and discussing other symptoms a person may be experiencing.
There are several different forms of angioedema with different underlying causes. It may be difficult to distinguish between the different types of swelling in some cases, and there isn’t a single test that can do so. Thus, a detailed review of symptoms along with specific lab tests may be needed to correctly diagnose the specific type of angioedema.
The importance of an early diagnosis
Swiftly and accurately identifying the cause and type of angioedema a person has is crucial because different angioedema types require distinct treatment approaches.
A quick and early angioedema diagnosis allows appropriate medication to be given as rapidly as possible to control the acute manifestations of the condition, and facilitate the adoption and implementation of strategies to prevent future swelling episodes.
For example, treatment of acute allergic angioedema generally involves the use of medications such as antihistamines to control the allergy, alongside preventive steps to limit future exposure to an allergen (a substance that can trigger an allergic reaction).
By contrast, hereditary angioedema is generally managed with medications that address its underlying genetic cause. Because swelling is not driven by an allergic reaction in these patients, antihistamines and other allergy medications will be ineffective in the management of this form of angioedema.
Symptoms and medical history
The first step in diagnosing and determining the underlying cause of angioedema is assessing a patient’s symptoms and reviewing their clinical and family history. A healthcare professional will generally be able to identify angioedema-like swelling, where fluid builds up in the deeper layers of the skin, by visual inspection.
Other angioedema symptoms that patients may experience alongside swelling include:
- redness, itching, or hives (urticaria)
- abdominal pain, nausea, or vomiting
- airway obstruction and difficulty breathing, which is a medical emergency and requires immediate treatment.
In addition to helping in an angioedema diagnosis, carefully assessing symptoms also may give doctors some hints to determine the type of angioedema a person has. For example, itching and hives are common signs of angioedema caused by an allergic reaction, but are less frequently observed in other forms of angioedema.
Assessing a patient’s medical history also can provide clues about the specific angioedema type. Clinicians typically will ask patients experiencing swelling if they have any history of asthma or allergies, and if they’ve recently been exposed to common allergens such as nuts or latex.
A healthcare provider also will review whether a patient is taking any medications that may cause angioedema as a side effect. If so, that medication will be stopped to see if swelling resolves, which can confirm the diagnosis of drug-induced nonallergic angioedema.
Whether a person has acute or chronic angioedema, with recurrent swelling episodes, will also help guide the diagnosis.
Finally, the patient’s family history also may support the diagnosis of a given angioedema type, as hereditary forms of angioedema usually affect multiple individuals in the same family.
Hereditary angioedema diagnosis
Hereditary angioedema, or HAE, is characterized by sudden bouts of swelling that occur as a result of a genetic mutation. The most common forms of HAE, known as types 1 and 2, are caused by mutations in a gene that provide instructions for making a protein called C1 esterase inhibitor (C1-INH). In type 1 HAE, those mutations result in a C1-INH protein that is missing or found at abnormally low levels; in type 2 HAE, the protein is present, but doesn’t work correctly.
People with HAE may experience swelling spontaneously in the absence of any clear trigger, or following certain triggers, such as stress, physical trauma, or infections. Swelling in HAE usually isn’t accompanied by hives, itching, or wheals, and it most commonly affects the face, extremities, genitals, digestive tract, or throat. Without treatment, swelling episodes usually last a few days and then subside.
If someone shows signs of HAE, such as recurrent swelling episodes, and/or has a family history of the disease, laboratory tests can be used to confirm the diagnosis.
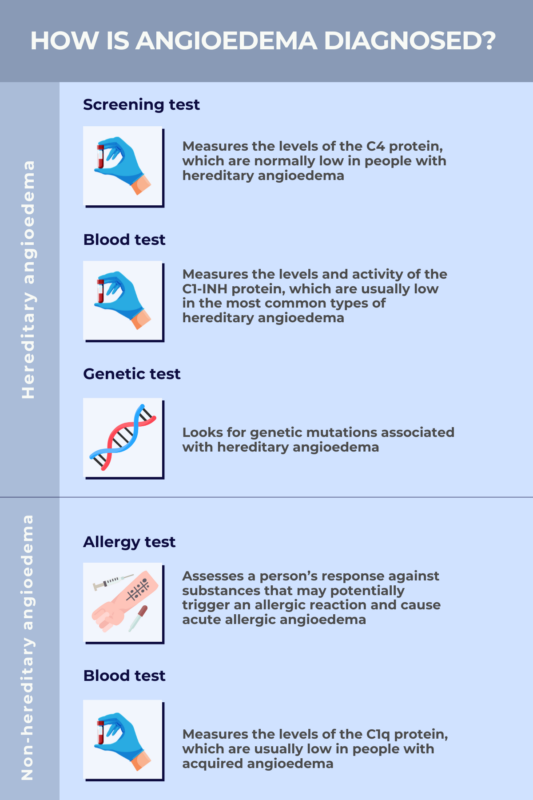
Screening test
Typically, the first angioedema test performed when someone shows signs of HAE is designed to measure the levels of a protein called C4 in the bloodstream.
The C1-INH protein that’s missing or is dysfunctional in HAE normally blocks the activity of an enzyme that breaks down C4. Because people with HAE types 1 and 2 have reduced C1-INH activity, they usually also have low levels of C4. Thus, measuring C4 levels can be a helpful screening test to point toward the possibility of HAE.
While this screening test can be useful, as many as 1 in 5 HAE patients will have normal C4 levels, even when levels are measured during swelling attacks. C4 levels also are typically normal in people with rarer types of HAE, so this screening test cannot definitively rule out HAE.
Blood test
Specialized blood tests to measure the levels and activity of the C1-INH protein also can be performed to help identify HAE types 1 or 2. Typically, tests measuring the levels of C4 and C1-INH, as well as C1-INH activity, are all run simultaneously if and when HAE is suspected.
In people with HAE type 1, the levels and activity of the C1-INH protein both will be low. People with HAE type 2 will have normal or high levels of the protein, but its activity will be low.
Genetic test
A diagnosis of HAE can be confirmed by genetic testing to identify the disease-causing mutation(s) a patient may be carrying. HAE types 1 and 2 are both caused by mutations in a gene called SERPING1. Thus, tests looking for defects in this gene can be used to confirm the diagnosis of these more common HAE types.
In rarer types of HAE, which are caused by mutations in other genes, genetic testing to look for other less common HAE-causing mutations is the only way to definitively make a diagnosis. In people who show signs of HAE, but have normal C1-INH levels and activity and no SERPING1 mutations, detailed genetic sequencing is recommended to look for potential disease-causing mutations in other genes.
Non-hereditary angioedema diagnosis
There are different diagnostic tests available to help clinicians identify the various forms of angioedema other than HAE.
Tests for acute allergic angioedema
If a patient shows signs of acute allergic angioedema, such as swelling that’s accompanied by itching or hives, clinicians will first try to determine whether there has been exposure to substances that may potentially trigger an allergic reaction. Then, once a potential allergen is identified, tests can be run to confirm the allergy. These may include:
- allergy tests like a skin prick test, where a tiny amount of the suspected allergen is used to poke the skin and see if it triggers a reaction
- blood tests to see whether the patient’s immune cells react against the suspected allergen.
Tests for acquired angioedema
Acquired angioedema is caused by a disruption in the function of the immune system that ultimately causes the levels and activity of the C1-INH protein to dip excessively low. It may be associated with autoimmune diseases or lymphoproliferative disorders — conditions where immune cells grow and expand more than normal. It may be caused by an autoimmune abnormality where a person’s immune system is driven to produce autoantibodies against C1-INH that prevent the protein from working normally.
Like people with HAE types 1 or 2, people with acquired angioedema usually have low blood levels of C4 and low C1-INH activity. However, individuals with acquired angioedema will typically have low levels of another protein called C1q in the bloodstream, which can help differentiate the two disorders. Anti-C1-INH antibodies may be found in some people.
Also, acquired angioedema is not caused by a genetic mutation, so genetic tests will not reveal noteworthy results in people with this type of angioedema, unlike in those with HAE.
Drug-induced nonallergic and idiopathic angioedema
In these two forms of angioedema, C4, C1-INH, and C1q levels are normal.
Drug-induced nonallergic angioedema is typically diagnosed when a patient is showing signs of angioedema after being exposed to a medication that can trigger the condition as a side effect. Idiopathic angioedema is diagnosed when a person experiences angioedema-like swelling, but its underlying cause cannot be identified. This is a diagnosis of exclusion, meaning the diagnosis is made by ruling out other potential explanations for angioedema.
Angioedema News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
Recent Posts
- HAE patients mostly attack-free after gene-editing therapy: Data
- Navenibart continues to reduce HAE attacks in long-term trial
- Adjusting eating habits to live better with HAE, other diagnoses
- Deucrictibant benefits maintained as treatment for HAE: Trial data
- FDA approves Andembry as preventive treatment for HAE
Related articles

 Fact-checked by
Fact-checked by 



