Orladeyo zeroes swelling attacks in HAE patients
Results from two clinical trials shared at annual AAAAI meeting
Written by |

People with hereditary angioedema (HAE) who took Orladeyo (berotralstat) for up to two years experienced no swelling attacks for most of the treatment duration, with fewer swelling attacks translating into a better quality of life.
That’s according to results from APeX-S and APeX-2, two clinical studies that evaluated the safety and efficacy of Orladeyo in people with HAE types 1 or 2.
Treatment-related side effects reported in both APeX-S and APeX-2 were mild and lasted only a short time, indicating that Orladeyo was generally tolerated well.
These findings were presented across two posters at the 2023 American Academy of Allergy, Asthma & Immunology (AAAAI) annual meeting, held Feb. 24-27, in San Antonio, Texas.
“The final results from the long-term APeX-S study show that Orladeyo was consistently well-tolerated, with no new safety signals observed, and attack reduction was sustained through 96 weeks [about two years],” Emel Aygören-Pürsün, MD, from the Department for Children and Adolescents of University Hospital Frankfurt, Germany, said in a press release.
People with HAE experience swelling attacks that can arise rapidly in any part of the body, such as in the face, throat, arms and legs, or around the gut.
BioCryst Pharmaceuticals’ Orladeyo is an oral medicine used to prevent swelling attacks in HAE. It is approved for people ages 12 and older, and works by blocking the activity of a protein called kallikrein.
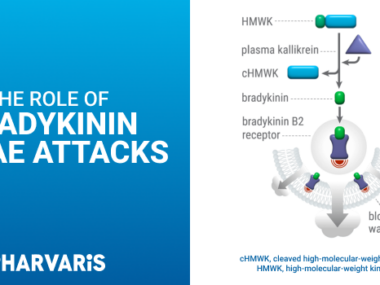
In HAE, overactive kallikrein triggers the overproduction of another protein called bradykinin. Too much bradykinin causes blood vessels to widen and become leaky, resulting in swelling. That’s how blocking the activity of kallikrein is expected to reduce the number of swelling attacks.
APeX-S (NCT03472040) was an open-label Phase 2/3 study in which patients were given one capsule containing either 110 mg or 150 mg of Orladeyo, once daily for up to 96 weeks (almost two years) in the U.S. and 240 weeks elsewhere.
Once it was found that the 150 mg dose worked better than the 100 mg, all participants were placed on the higher dose. Of the 387 people who took part in the study, 287 received the 150 mg dose for the entire duration of the study, while 100 initially received the lower 110 mg dose.
In those who were always on the higher dose, swelling attacks dropped from a mean of 1.1 in the first month to 0.8 in the last month of treatment. A median of zero swelling attacks was observed for most of the treatment duration (20 of the 24 months).
Sustained reduction in attacks
“Patients experienced a sustained reduction in attacks throughout treatment,” researchers wrote in the poster abstract. “These final results from APeX-S support the long-term safety and efficacy of oral berotralstat, making it an effective and convenient prophylactic [preventive] HAE therapy option.”
The abstract, “Long-term HAE Prophylaxis with Berotralstat Is Well Tolerated and Effective: Analysis for the APeX-S Study,” was published in the Journal of Allergy and Clinical Immunology.
Treatment-emergent side effects occurred in 334 (86.3%) patients, the most common being an inflammation of the nose and throat (23.8%), followed by headache (14.7%) and diarrhea (14.5%).
Side effects related to the medicine occurred in 177 (45.7%) patients, with four experiencing a serious treatment-related side effect. Side effects caused 36 (9.3%) patients to stop treatment.
In the placebo-controlled Phase 3 study ApeX-2 (NCT03485911), Orladeyo was found to bring about a better quality of life in a group of 40 people who were on the 150 mg dose for up to 96 weeks.
Assessment tool
Changes in quality of life were measured using the patient-reported Angioedema Quality of Life Questionnaire, where lower scores indicate better quality of life. The minimal clinically important difference was defined as a six-point reduction in the total score.
Improvements exceeded the minimal clinically important difference starting at week 4, and were sustained through the end of the study. There was a drop of at least 18 points regardless of age, sex, prior swelling attack rate, prior treatment, or presence of gastrointestinal side effects.
“Long-term prophylaxis with berotralstat led to sustained and clinically meaningful improvements in patient-reported [quality of life], across multiple subgroups, suggesting sustained reductions in disease and treatment burden,” the researchers wrote in another poster abstract.
The abstract, “Berotralstat Improved Quality of Life through 96 Weeks Across Multiple Subgroups of Patients with Hereditary Angioedema,” was published in the same journal.
These positive findings also were strengthened by real-world data analyses on the use of Orladeyo.
A third poster abstract, “Real-World Outcomes in Patients with Hereditary Angioedema (HAE) Treated with Berotralstat,” reported data from 213 patients who took the medicine for at least 120 days.
Swelling attack rates dropped from a median of 1.67 to less than 0.5 attacks per month in about three-quarters of the reporting periods out to 360 days (nearly one year) on treatment.
Real-world evidence
“This real-world evidence supports the continued need for an oral, once-daily option for patients and physicians who are seeking control of their HAE attacks,” said Ryan Arnold, MD, BioCryst’s chief medical officer.
Studies are underway to test Orladeyo in children ages 2-11 years. Another poster abstract titled, “Disease and Treatment Burden of Hereditary Angioedema (HAE) in Pediatric Patients: Assessment by Caregivers,” reported findings from an online survey where adults caring for children with HAE were asked to share their experiences with available treatments.
It was found that fewer than one in five children were on preventive treatment for HAE. Treatment infusion requirements and inconvenient administration were cited as the most common reasons why children were not on preventive treatment. Additionally, almost half (40%) of the caregivers reported at least one swelling attack in the previous six months.
“Pediatric patients experiencing attacks may not be receiving HAE treatments due to worry over burden of treatment, highlighting the need for a new oral treatment option,” the researchers wrote in that poster abstract.