Angioedema due to blood pressure meds can raise cardiovascular risk
Study calls for close monitoring of ACE inhibitor-induced angioedema
Written by |

People who develop angioedema due to common high blood pressure medications known as angiotensin-converting enzyme (ACE) inhibitors may be at an increased risk of a cardiovascular event in the few months after discontinuing treatment, a study has found.
While it’s not clear if switching to an alternative treatment may reduce that risk, this finding calls for the need to closely monitor patients and adjust their medication regimen.
“Future studies should assess the role of early initiation of alternative medications after an episode of [ACE inhibitor]-related angioedema,” researchers wrote.
The study, “Cardiovascular Outcomes After Angiotensin Converting Enzyme Inhibitor Induced Angioedema: A Retrospective Cohort Analysis,” was published as a brief report in The American Journal of Cardiology.
ACE inhibitors used to lower blood pressure, improve heart health
ACE inhibitors are commonly used to lower blood pressure and improve heart health. They work in part by increasing the level of bradykinin, a substance that helps widen and relax blood vessels.
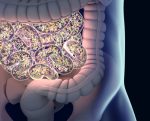
However, bradykinin can also cause fluid to leak from blood vessels into nearby tissues, resulting in swelling, or angioedema. While rare, non-allergic angioedema can occur as a side effect of ACE inhibitors.
When people experience ACE inhibitor-induced angioedema, they may stop taking their medication. However, it’s not known if this increases their risk of developing cardiovascular conditions in the future.
To know more, researchers looked at data from 600 people, with a median age of 58 years, who were admitted to the hospital after an episode of angioedema. In 363 (61%) of them, angioedema was caused by an ACE inhibitor.
Most (82%) were taking an ACE inhibitor to treat hypertension (high blood pressure), and about half (52%) were taking the medication for chronic kidney disease, which occurs when the kidneys stop working over time. Other indications for taking ACE inhibitors included diabetes and heart failure.
People with ACE inhibitor-induced angioedema were older (median of 60 years) than those with angioedema due to other causes (53 years). They also were more likely to be African-American (93% vs. 86%) and to have hypertension (99% vs. 57%) and diabetes (40% vs. 28%).
Everyone who experienced ACE inhibitor-induced angioedema stopped taking their medication, but for nearly 64% of them, an alternative wasn’t provided.
Others were started on calcium channel blockers (21%), thiazide diuretics (12%), or beta-blockers (7%), among other types of medications. Six (2%) were started on angiotensin receptor blockers, “despite having continued indications for these medications.”
A median of 119 days (nearly four months) after their episode of angioedema, 47 (8%) people experienced a cardiovascular event. Nearly half of these events (45%) occurred within the first three months.
Cardiovascular events included sudden, severe high blood pressure
The most common types of cardiovascular events were a sudden, severe increase in blood pressure in 20 (43%) people, followed by acute coronary syndrome, or a decrease in the blood flow to the heart, in 12 (26%).
A worsening of heart failure occurred in eight (17%) people. Five (11%) experienced a stroke or a transient ischemic attack, where the blood flow to the brain is blocked, and two (4%) had other types of blood vessel-related events.
People with ACE inhibitor-induced angioedema were more likely to experience a cardiovascular event (10%) than others with angioedema due to other causes (4%). It also was more common for them to have recurrent cardiovascular events (5% vs. 1%).
Overall, these patients were 2.67-times more likely to experience a cardiovascular event.
“This increased risk is likely multifactorial,” the researchers wrote, adding that “[ACE inhibitor] discontinuation may be a contributing factor.”