C1 Inhibitor Use May Safely Prevent HAE Attacks in Pregnant Women
Written by |

Subcutaneous (under-the-skin) administration of human plasma-derived C1 inhibitor is an effective and safe option for managing hereditary angioedema during pregnancy and lactation, a case report suggests.
The study, “Subcutaneous C1‐Inhibitor Concentrate for prophylaxis during pregnancy and lactation in a patient with C1‐INH‐HAE,” was published in the journal Clinical Case Reports.
HAE is a rare genetic condition mainly caused by mutations in the gene that holds the instructions for the C1 inhibitor (C1-IHN) protein. In HAE type 1, such mutations significantly lower the levels of C1-IHN.
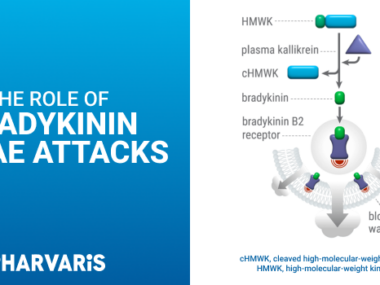
In the absence of enough C1-INH, levels of the inflammatory molecule bradykinin rise, causing blood vessels in the deep layers of the skin to widen. This allows fluid to escape into surrounding tissues, causing swelling.
Clinical management of HAE is particularly challenging during pregnancy, which increases estrogen levels. Estimates suggest that about 60% of women with HAE experience a worsening of attacks during pregnancy.
Moreover, most medicines to prevent or treat HAE attacks are not indicated for use during pregnancy and lactation. These patients are usually offered plasma-derived C1-IHN — which replenishes blood levels of C1-IHN — as an on-demand treatment for acute swelling attacks, and tranexamic acid to prevent attacks.
Researchers at Goethe University Frankfurt am Main, in Germany, reported the case of a 38-year-old woman with type 1 HAE, who was successfully treated with plasma-derived C1-IHN as a prophylaxis, or treatment given to prevent swelling attacks, while she was pregnant and nursing.
The woman had been diagnosed at age 17, and had a history of mild disease. She experienced an increase in attack frequency when she began an estrogen contraceptive pill, but attacks dropped to less than two a year after she was prescribed a progesterone-only pill. Attacks at this time were treated with 500 to 1000 units of C1-IHN administered intravenously (directly into the bloodstream).
After she stopped all hormone contraceptives, planning for a pregnancy, her attacks increased to four per year. During the first two months of the pregnancy, the frequency of attacks rose further, to two or three each month. Treatment was given for severe attacks only.
She continued to experience swellings on a daily basis, as well as swelling in different parts of the body simultaneously, which significantly affected her quality of life and led to symptoms of depression.
After being hospitalized due to xserious swelling in the throat, both the patient and her husband were trained to administer C1-IHN intravenously at home, to treat attacks rapidly.
Attack frequency continued to increase, reaching twice a week at end of the pregnancy’s second trimester. Because vein access was now compromised, clinicians decided to give the woman preventive subcutaneous injections of C1-IHN, at 1500 units twice a week. She was also trained to administer these injections at home.
This preventive treatment stopped the attacks through delivery of a healthy child at 38 weeks of gestation. She continued with the subcutaneous injections after the birth, and one month later also resumed oral progesterone.
Within seven weeks, the treatment was reduced gradually, to once weekly injections for one month. But an interruption in these injections for eight days resulted in foot swelling. She restarted treatment once a week for three more weeks.
New swellings in the throat, foot, and elbow, however, led her to return to her twice-weekly treatment. She remained without swellings almost for 10 months after delivery on this therapy schedule.
After that time, she developed swelling in the mouth and throat due to stress, and shortness of breath. She received treatment with intravenous C1-IHN in the hospital, but continued to have recurrent symptoms in the following weeks.
Because the swelling was affecting the throat, a critical site, her twice weekly preventive dose of subcutaneous C1-IHN was increased to 60 units per kilogram of body weight. The patient remained attack free with this approach.
Overall, this case suggests that subcutaneous C1-IHN administration “is a successful and safe treatment option for prophylaxis in [type 1 HAE] during pregnancy and lactation, and may be effective in less than recommended doses over long periods of time,” the researchers wrote.
“This case also adds to the clinical evidence of safety and efficacy of subcutaneous C1‐INH for prophylaxis in HAE,” they added.