Cholesterol-lowering Atorvastatin Linked to Angioedema for 1st Time
'Statins cannot be disregarded as the primary or contributing cause of angioedema'
Written by |
Atorvastatin, a cholesterol-lowering medication, has been linked to angioedema for the first time in a recent case report, highlighting the need for comprehensive evaluation of all medications taken by patients, regardless of their medical history.
“Statins cannot be disregarded as the primary or contributing cause of angioedema,” researchers say.
Their case report, “Atorvastatin as a Rare Primary Cause of Drug-Induced Angioedema: A Case Report,” was published in the journal Cureus.
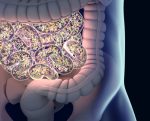
Angioedema, a condition characterized by swelling in the deeper layers of the skin, can be caused by several factors, including medications. In fact, an estimated 32% of angioedema cases are triggered by certain medications.
Angiotensin-converting enzyme inhibitors — a class of medicines to treat high blood pressure — are among the most well-known medications that can trigger angioedema. They increase the levels of bradykinin, which is a molecule that causes blood vessel widening and fluid leakage — leading to tissue swelling, the main symptom of angioedema.
Statins are widely prescribed to lower cholesterol levels in the blood and reduce the risk of stroke, heart attack, and other heart complications, but their use has not been linked to angioedema.
This report describes the case of a man who developed angioedema after taking atorvastatin, a statin sold under the brand name Lipitor, among others.
Case report of Asian man, 59, diagnosed with high cholesterol
The patient, a 59-year-old Asian man, had been diagnosed with hyperlipidemia — a condition characterized by the presence of abnormally high levels of fatty molecules (lipids) in the bloodstream — and went to his primary care physician for treatment. His family history included heart disease and high cholesterol.
He was otherwise healthy, did not have high blood pressure or diabetes, and was not taking any medications. He had no history of allergies to medications or foods, and had not experienced adverse hypersensitivity reactions in the past.
After examination, he was prescribed atorvastatin (40 mg dose) for his hyperlipidemia, and advised to exercise regularly and follow a healthy diet.
Within hours of taking atorvastatin, he developed numbness and swelling of the tongue and face. Despite these symptoms, he continued taking the medication for a few days. These episodes were recurrent and became increasingly more severe over time.
He was brought to the clinic for evaluation, which confirmed he had facial numbness and swelling, but no rash or itchiness. His tongue was mildly swollen, but he had no problems breathing and swallowing.
Physicians suspected angioedema and started the patient on into-the-vein infusions of prednisolone, a steroid used to reduce inflammation. After 24 hours, the swelling resolved without the need for additional steroid treatment.
A re-evaluation of his medical history revealed no swelling, hypersensitivity reactions, or food allergies. Also, the patient had not eaten anything unusual nor had he traveled recently. His blood tests also came back normal.
His medication use was reviewed and treatment with atorvastatin “was found to be the primary cause for such recurrent angioedema, as these episodes occurred only after oral statin intake,” the researchers wrote.
The patient was then diagnosed with statin-induced angioedema, and began treatment with ezetimibe (sold as Zetia, among other brand names), another cholesterol-lowering medication that has a different mode of action than statins, for his hyperlipidemia.
At a follow-up one week later, the patient did not report any angioedema-like episodes.
“Drug-induced side effects may indicate the need for a comprehensive evaluation of all the patients’ medications,” the researchers wrote.
“The immediate withdrawal of the suspected drug(s) and treatment … should be the primary goal to prevent the severity of angioedema,” they added.